|
|
Kratom
Kratom is a South-East Asian plant with tallness that reaches from 4 to 16 meters. The leaves of this superb tree have one-of-a-kind properties that make them useful for different conditions like improving temperament, easing torment, energy-supporting, and assisting individuals with conquering laziness and weariness. Kratom is accessible in various structures and in case you’ve been thinking about what amount of time kratom containers require to kick in, unwind as this article is for you.
Kratom Capsules
Crazy Kratom capsules are acquiring ubiquity across the world, yet have you at any point asked yourself what they are? Indeed, they are kratom powder that has been pre-stuffed into capsules. Producers measure the right amounts and fill them in the covers, which you purchase and take with water.
Sorts of kratom capsules
Before we let you know what amount of time it requires for the kratom case to kick in, we […]

Living in an age where quantity is easily available but the quality is compromised, we need to be extra cautious with our choices. Our negligence becomes a problem when it comes to the herbs and medicines that have a direct impact on our well-being. Considering these reasons, people prefer to shop from renowned stores like Walmart.
Walmart is the largest company in the world in terms of revenue. It is basically an American chain of grocery stores as well as retail departments. Being a family-owned business, it was founded in 1962 and now it is widely known across the globe.
Although Walmart has a vast array of consumer products, some people, especially Kratom-heads end up thinking, Will I be able to find Kratom at Walmart? Don’t worry! We can have it answered for you. All you gotta do is to stick with us till the end!
What Is Kratom?
Mitragyna […]

Inevitably, Kratom is a botanical on which plenty of people rely for years. It has been helping them to combat some health issues. However, this is not enough to make it available at all famous stores. Can’t guess what we are talking about? Let us make it clear.
General Nutrition Centre which is also known as GNC is U.S based but it has its branches almost all across the world. The widely spread branches speak for its popularity. Although it has all the minerals, vitamins, and supplements, the question remains, Is it possible to buy Kratom from GNC? To find a clear-cut answer to this and a lot more related queries, keep reading the article!
What Is Kratom?
Kratom which is also commonly known as Crazy Mitragyna Speciosa is a herb. It serves medicinal and recreational purposes. Being available in a number of forms, this herb is segregated in the […]

Are you one of those people who feel under the weather because of the complications life is offering? If yes, you might have thought about getting your hands on a safe yet effective herb to help you go through all these ups and downs.
Kratom, which is also known as Mitragyna Speciosa, is one of such herbs but it is not that you go to the market and buy it right away. Certainly, it is available online as well as in the stores but Kratom comes in different types, strains, and also in the form of different products. As its demand has increased, now a number of companies are adding it to their product range. Already feel confused? Well, we have gathered for you some important information to make you familiar with the different types of Amazing Kratom being available in the market. So, let’s begin!
Popular Kratom Strain Types […]

What happens when you don’t take kratom in moderation and get used to overdosing? The answer is pretty obvious; you fall into kratom sickness, also known as kratom hangover. Kratom sickness is an extremely unpleasant state and one should be watchful about it ahead of time.
Whether you want to be preventive against kratom sickness or you have experienced it and want to know how you can get rid of it, this piece is all you need to read. From the causal factors to tips and tricks to control kratom sickness, we will catch a glimpse of every essential detail.
What is Kratom Sickness?
Kratom sickness is a result of consuming higher dosages of kratom. Remember, your body is used to a certain dose of kratom. When all of a sudden, you increase that dose to 2x or 3x, it responds differently. The user experiences exhaustion, nausea, s spinning head, […]
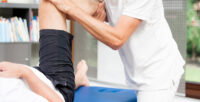
Arthritis is not at all an easy disorder to suffer from. Where it introduces pain to your joints and bones, there it also makes it difficult for you to perform daily tasks. Without giving it any consideration, it can even advance to another severe disorder, named Osteoarthritis. Anyway, there have been many treatments available for this health condition but the majority of them only help in reducing the pain levels.
As we all know, allopathic treatments are pretty much avoided since the beginning. One of the reasons behind this hesitance is the fact that allopathic treatments carry far more side effects than homeopathic treatments. Secondly, homeopathic treatment and medication are pretty much pocket-friendly. Are these not some big reasons to settle for?
Fortunately, there are plenty of herbs available in front of you to choose from and lately, Crazy Kratom is gaining mass attention to serve the purpose. Many people […]
|
|







